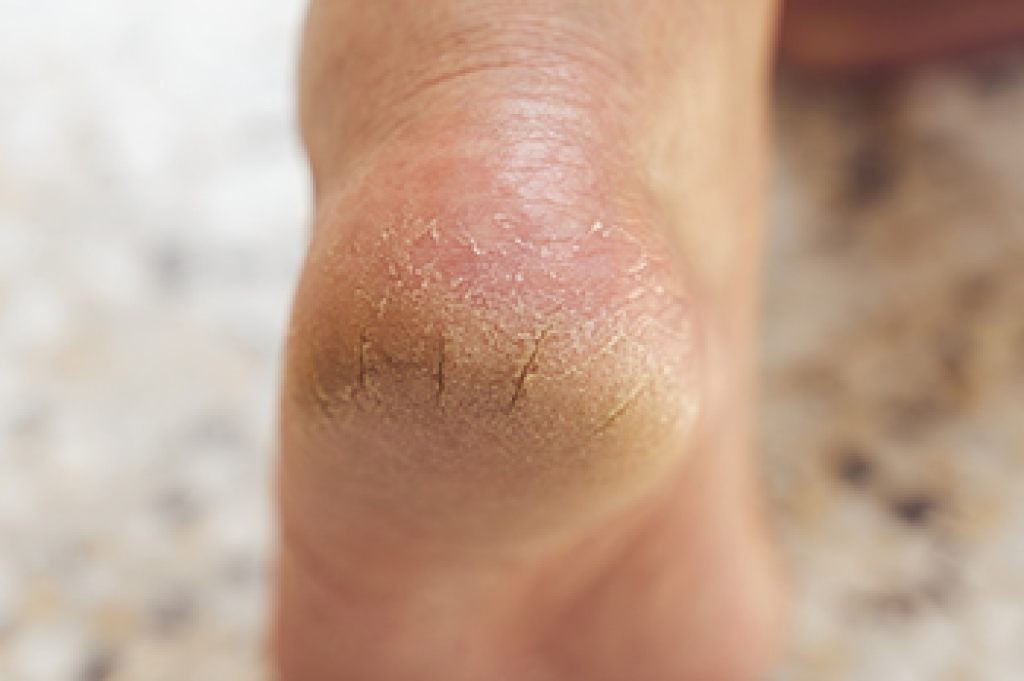
Cracked heels occur when the skin on the heels becomes dry, thick, and hardened, eventually splitting under pressure. This often develops from standing or walking on hard surfaces for long periods, which places extra stress on the heel. Being overweight can also increase pressure and contribute to skin breakdown. Symptoms include rough skin, visible cracks, and discomfort while walking. Risk factors include poor hydration, lack of foot care, and wearing open back shoes that do not provide support. A podiatrist can remove thickened skin, recommend moisturizing treatments, and provide guidance to prevent worsening of the condition. If you have developed painful cracked heels, it is suggested that you consult a podiatrist who can effectively treat this problem.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Brian Doerr, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Fort Meyers, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.